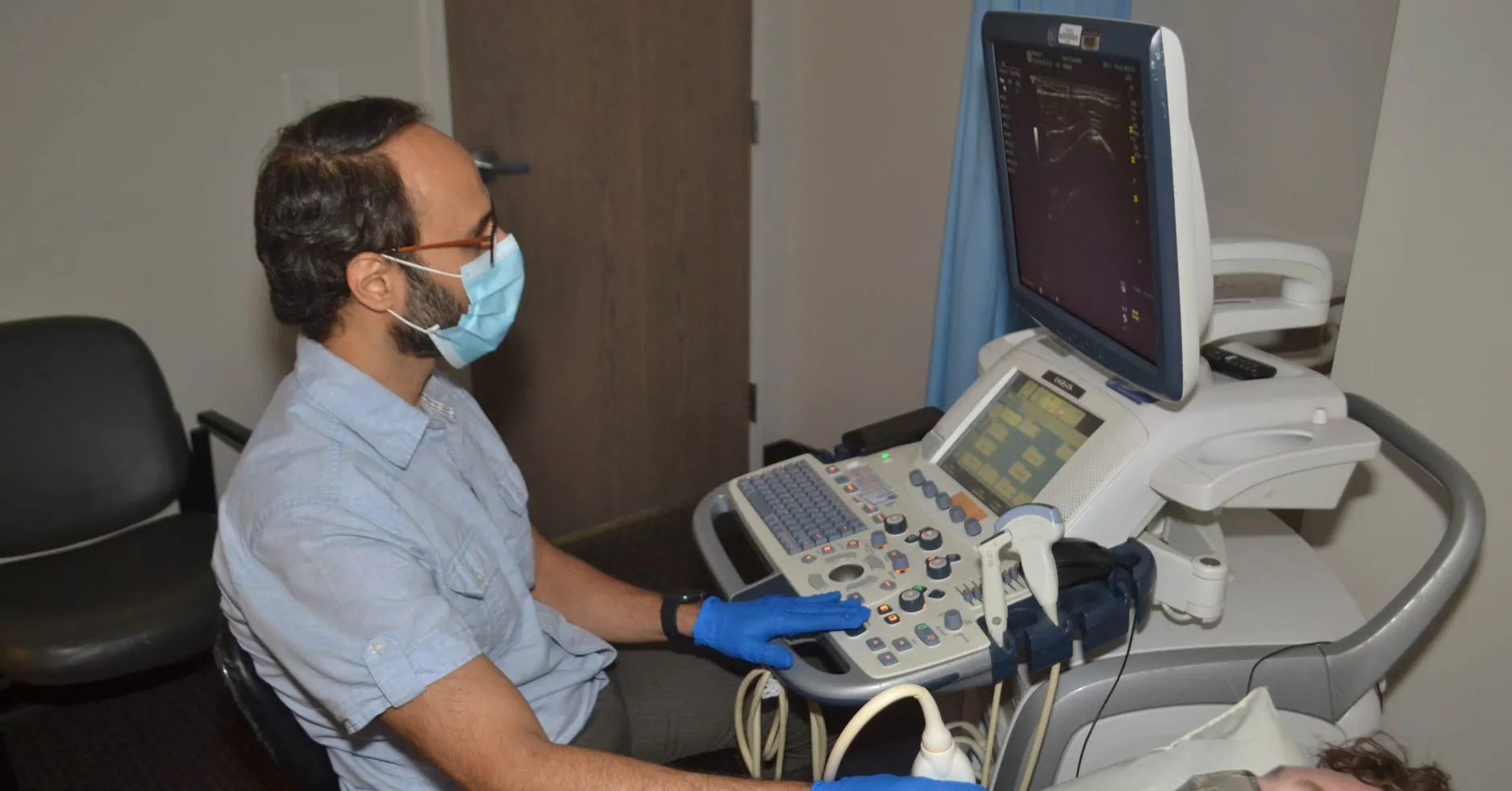
The advanced, targeted use of biologics centers on a patient-specific model of care.
LEXINGTON Platelet-rich plasma (PRP) has rapidly evolved from a niche intervention into a widely adopted tool across orthopedics, sports medicine, and interventional pain practices. Its appeal is intuitive: a biologic therapy derived from the patient, with the potential to modulate inflammation and support tissue repair. As utilization has expanded, however, so too has variability in outcomes — prompting a broader reconsideration of how PRP is best understood and applied.
What has become increasingly clear is that variability in outcomes is less about PRP itself and more about how precisely it is applied.
At Wellward Medical, this evolution was driven in part by a growing dissatisfaction with the traditional trajectory of musculoskeletal care. Too often, patients cycled through a revolving door of treatments — medications, injections, and temporary relief — without a clear path toward meaningful recovery. In many cases, this created a system in which patients became dependent on ongoing interventions rather than progressing toward autonomy. Since 2012, Wellward has intentionally shifted away from predominantly palliative approaches toward regenerative strategies — including PRP — aimed at changing the trajectory of care toward functional independence.
Within this framework, PRP is not simply an injection. It is a strategy — one that depends on diagnostic precision, structural targeting, and integration into a more comprehensive model of care. This model, developed and refined at Wellward, centers on combining advanced diagnostics with structure-specific biologic treatment to address the underlying drivers of joint dysfunction.
In many clinical settings, PRP is delivered as a discrete procedure, often as a single intra-articular injection for symptomatic joints such as the knee or shoulder. This approach can provide meaningful symptom relief and remains appropriate in selected cases. However, experience across hundreds of patients treated at Wellward — spanning the spine, knees, hips, shoulders/rotator cuff, and smaller joints — suggests that PRP functions less as a stand-alone intervention and more as a platform therapy, with outcomes highly dependent on how and where it is deployed.
Identify, Then Treat
This distinction becomes most apparent when evaluating the drivers of joint pain. Traditional models often center on intra-articular pathology — cartilage degeneration, synovitis, or labral injury. While important, these findings frequently represent only one component of a broader biomechanical problem. Many patients also exhibit ligamentous insufficiency, capsular laxity, tendinous dysfunction, or impaired neuromuscular control — factors that contribute to joint instability and progressive degeneration.
At Wellward, identifying these contributors is central to treatment planning. High-resolution musculoskeletal ultrasound (MSKUS) serves as a dynamic extension of the physical examination, enabling real-time assessment of joint stability and precise correlation with symptoms. This often reveals that what appears to be isolated joint disease is part of a more complex functional disturbance.
Reframing the Target: From Inflammation to Stability
Within this framework, joint degeneration is not viewed solely as cartilage wear, but often as a consequence of compromised stability. Even subtle laxity in ligamentous or capsular structures can alter load distribution, increasing stress on articular surfaces and perpetuating degeneration.
This perspective expands the therapeutic role of PRP. Rather than functioning only as an intra-articular biologic adjunct, PRP can be applied to support stabilizing structures — ligaments, entheses, and capsular tissues — helping restore balance within the joint as a functional unit.
While intra-articular PRP remains a valuable approach, treatment at Wellward frequently extends beyond the joint space. Using MSKUS guidance, PRP is delivered to periarticular structures contributing to instability. In this way, treatment is not simply placed — it is precisely matched to the structures most responsible for dysfunction.
From Single Injection to Coordinated Care
A parallel shift has occurred in how PRP is incorporated into care. Rather than a one-time intervention, it is increasingly used as part of a longitudinal strategy.
At Wellward, PRP is integrated with rehabilitation, load management, and broader physiologic factors that influence healing. In selected cases, treatment is staged in alignment with biologic repair timelines. The emphasis is not on increasing procedural volume, but on aligning interventions with structural and functional needs over time.
Joint disease does not occur in isolation. Mechanical stress, activity patterns, and systemic factors all influence outcomes. Addressing these alongside targeted biologic therapy allows for a more complete and durable response. Patients often respond not only to the intervention itself, but to the clarity of diagnosis and the sense that care is tailored to their condition.
Clinical Vignettes: Expanding the Lens of Treatment
This model frequently changes both diagnosis and intervention.
In knee osteoarthritis, for example, evaluation may reveal contributing factors such as ligament laxity or tendon dysfunction. Addressing these alongside intra-articular pathology can improve stability and clinical outcomes.
Similarly, in shoulder pathology, treatment may extend beyond the joint to include the rotator cuff, biceps tendon, and capsular structures that influence stability.
A similar principle applies in the spine. A patient presenting with chronic low back pain attributed to disc degeneration and facet arthropathy was found to have underlying ligamentous hypermobility and listhesis. Rather than targeting only the disc or facet joints, treatment focused on stabilizing the functional unit using PRP directed at ligamentous support, combined with bone marrow aspirate concentrate (BMAC) to address disc degeneration. Over a series of treatments, the patient reported improved stability with movement, increased walking tolerance, and a significant reduction in the deep, activity-limiting pain that had previously worsened with standing. While surgical intervention remains a future consideration, the trajectory has shifted meaningfully, with surgery becoming a more distant — and potentially avoidable — option.
The Ideal PRP Patient
In practice, this approach is particularly relevant for patients who fall into a therapeutic gap — those seeking to preserve joint function rather than react to decline. This includes active individuals aiming to prevent or slow degenerative changes, patients considering surgery who wish to optimize outcomes or explore alternatives, and those with persistent pain despite physical therapy or prior injections. It is especially impactful in early to moderate degeneration, where joint preservation remains a realistic goal and earlier intervention may meaningfully influence long-term trajectory.
Although PRP has demonstrated meaningful clinical benefit and potential downstream cost savings, insurance coverage has not kept pace with its evolving role. Ongoing advocacy efforts aim to address this gap. In the interim, practices such as Wellward prioritize access through flexible payment structures and by offering a spectrum of alternative options when regenerative care is not financially feasible.
Variability in PRP outcomes is well recognized. While preparation methods and patient selection play a role, target selection — what structures are treated and why — may be an equally important and underappreciated factor.
Evidence remains heterogeneous, though meta-analyses suggest benefit in knee osteoarthritis and select tendinopathies, particularly in earlier disease. It is equally important to recognize that PRP is not universally effective; advanced degeneration or structural limitations may reduce response. A diagnostic-first approach helps clarify when biologic strategies are appropriate and when alternative pathways, including surgery, may be more beneficial.
Across a broad clinical experience, most patients treated within this framework report meaningful improvement. While PRP is not a restoration to a younger joint, internal registry data at Wellward demonstrate high patient satisfaction, with approximately 95% of patients reporting they would pursue the treatment again and recommend it to others.
Conclusion
The question surrounding PRP is no longer simply whether it works, but how it is best deployed.
Outcomes appear optimized when PRP is guided by detailed diagnostics, targeted to both intra- and periarticular structures, and integrated into a broader strategy. Approaches such as those implemented at Wellward reflect this shift — moving beyond isolated injections toward a more precise, structured, and patient-specific model of care.
For referring clinicians, this approach can provide a meaningful option for patients seeking to preserve function while delaying or refining the timing of surgical care.
As musculoskeletal medicine continues to evolve, this transition from injection to strategy may define the next phase of non-surgical joint preservation — one centered on precision, structure, and long-term function.