Elizabeth Bruenderman, MD, UofL Health bariatric surgeon, helps patients win their weight loss battles
LOUISVILLE When someone is at the end of their rope and you hand them a lifeline, that’s a heroic gesture. Those lifelines can be big or small, the size doesn’t matter; it’s the courageous act of offering, and accepting, the lifeline that counts.
For many people, their fight against obesity is filled with failures and some success, says Elizabeth Bruenderman, MD, medical director of the Advanced Bariatric Surgery and Weight Loss Center at UofL Health. She says the solution for weight loss of eating less and exercising more oversimplifies and underestimates the challenge of meaningful weight loss.
“Historically, patients were blamed for their weight,” Bruenderman says. “We know based on science and the biology of the disease that obesity is much more complex than just calories in and calories out. The interactions that are at play are some of the most complex and misunderstood biological processes.”
Growing up in Louisville, understanding the complex obesity problem was not on her radar. Bruenderman was active in sports, including rowing and swimming at Sacred Heart Academy. She graduated from George Washington University in Washington, DC, with a degree in economics.
Bruenderman, however, was exposed to the medical field at an early age by her father David Bruenderman, MD, a now-retired anesthesiologist. She was drawn back to Kentucky and a career in medicine. She went to the University of Louisville School of Medicine, then completed a general surgery internship and residency at UofL before taking a minimally invasive bariatric surgery fellowship at Duke University in 2023. Upon completing the fellowship, Bruenderman was back at UofL Health, where she helped launch the bariatric program.
“I was not planning on becoming a surgeon, but when I did my clinical rotations as a third-year medical student, I pretty much loved every minute of my surgery rotation,” Bruenderman says. “No other rotation compared to it, and it was obvious that this was the choice for me. I liked the idea of surgery having a very palpable result. I find that very satisfying.”
The Bariatric Patient
Bruenderman finds joy and purpose in helping people in her hometown and takes pride in being the only female bariatric surgeon now practicing in Louisville. Eighty percent of bariatric surgery patients nationally are female, and Bruenderman’s patients range in age between 18 to 75 and older.
“It’s a different relationship that you have between two women when you’re talking about a topic as sensitive as weight,” Bruenderman says. “I think that makes a really big difference for my patients, their comfort level, and our ability to understand each other.”
Bruenderman says that for many patients, bariatric surgery is their last resort. Perhaps they have tried diets, lifestyle changes, and weight loss medications, but with little or no long-term success. That’s when they come to see Bruenderman.
“They are, by and large, at the end of their rope and have done everything except surgery,” Bruenderman says of her bariatric surgery patients. “People see surgery as a last result even though it is a very safe and the most effective option for weight loss.”
Helping patients understand the surgery is part of her initial meeting with patients. Bruenderman says these first meetings average about 45 minutes as she learns as much about the patient’s history and goals as possible. She explains to her patients their options, both surgically and medically, and gains an understanding of the patients’ goals.
“I don’t ever decide for the patient,” says Bruenderman, who says that 80 percent of her work is bariatric surgery. She also does endoscopies and general surgery. “We talk about it and come to a conclusion together. The benefit we have in the weight loss clinic is that if they decide they want to try medical therapy first, all of that is done here under one roof.”
That’s important not only because of the multiple ways in which obesity can be treated, but also because it allows an open conversation between physicians, colleagues, and patients. Everyone is on the same page with the same goal.
“What we seek to do is to view obesity as a disease, as something that is incredibly complex that patients need lifelong counseling on,” Bruenderman says. “This is a chronic condition. The medical field has been very slow to accept that.”

The New Weight Loss Paradigm
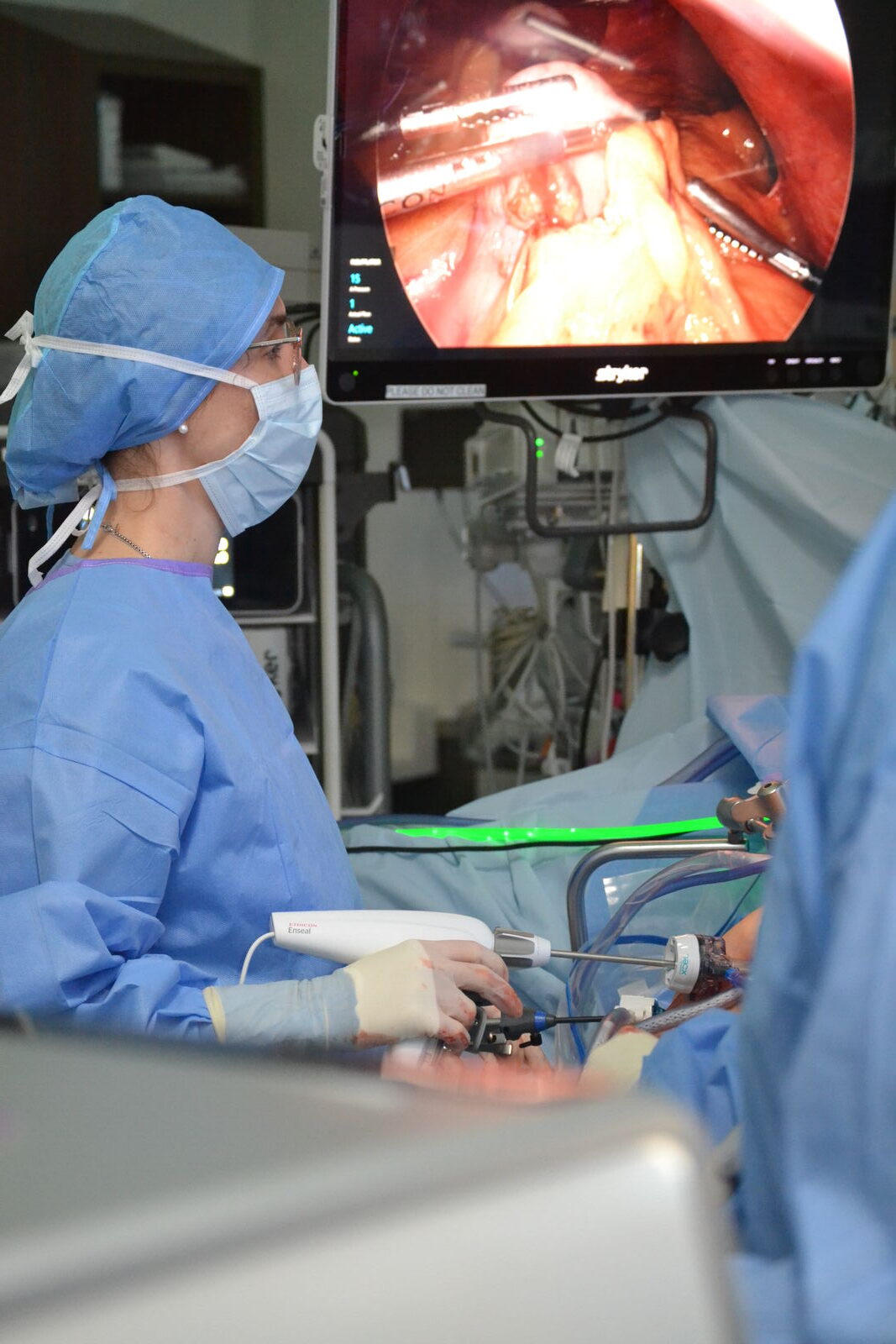
Diet and exercise are now joined by bariatric surgery and GLP-1–based medications as powerful tools to treat and manage chronic obesity. At Bruenderman’s clinic at UofL Health, patients receive integrated care that includes bariatric surgery, anti-obesity pharmacotherapy, endoscopic procedures, and dietitian support, with close collaboration with behavioral health specialists and attention to sleep as a key component of metabolic health.
“We are a comprehensive center to treat weight. That means you may see a surgeon, you may see a medical weight loss provider, you might see a dietician, a GI interventional endoscopist, or all of the above,” Bruenderman says.
“Everyone in our clinic is hyper-focused on helping patients through this process and making sure that patients feel they can come to us in any state, in any condition, with any kind of attitude or motivation level. We can help them and we want to help them.”
Bruenderman says patients who have not had the success losing weight that was expected are often reluctant to come back to their physicians for fear of being considered a disappointment or failure. Changing that mentality is a primary focus for Bruenderman and those on her team.
“People get into this negative feedback loop where one condition begets the other. To make meaningful changes in your life with diet and exercise alone, you have to make maximal changes to your lifestyle, and that process is a very slow one that has a lot of ups and downs associated with it,” Bruenderman says. “I have the tool, bariatric surgery, that is known to reverse all that in the most significant and durable way. It is very profound to see how much of a difference it makes in every aspect of someone’s life, giving them this jumping off point to start seeing maximal changes from their efforts.”
Not Your Aunt’s Bariatric Surgery
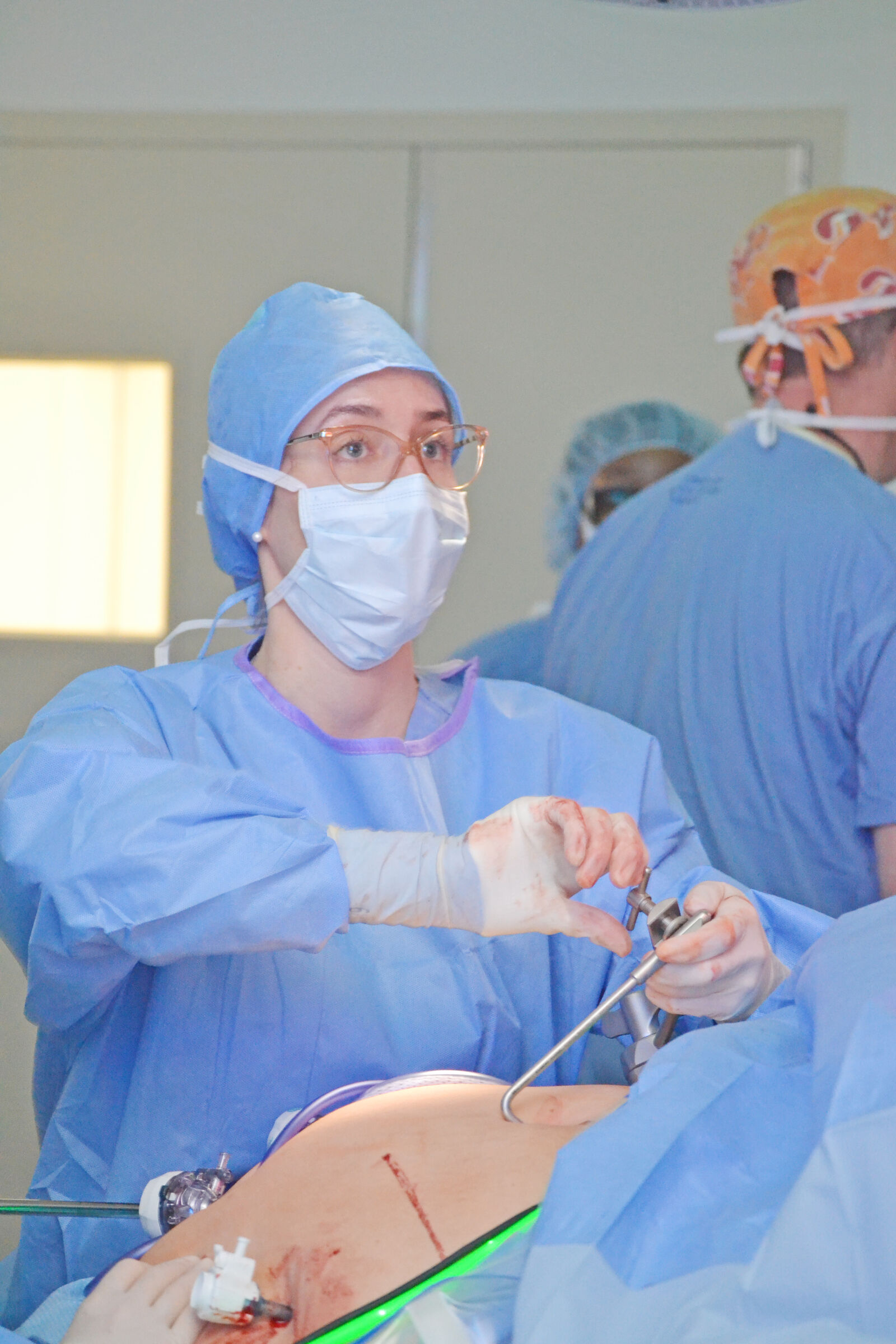
The field of bariatric surgery is between 60 and 72 years old, with the first gastric bypass surgery performed in 1966. Bruenderman notes that bariatric surgery has evolved significantly over the past 15 to 20 years. Many people who had bariatric surgery before then, or knew someone who did, are skeptical because poor outcomes were much more frequent. She points to minimally invasive laparoscopic surgery as one of the primary reasons for improved outcomes in recent years, as well as new and improved bariatric procedures and more stringent quality standards.
“Bariatric surgery is now as safe as very commonly performed surgeries such as having a gallbladder removed or having a hysterectomy,” Bruenderman says. “The gastric bypass that your aunt got 15 years ago is not the same one that you’re getting today. Our preoperative patient pathways and postoperative care algorithms ensure the surgery is going to be as safe as it can possibly be and set patients up for long term success.”
The gastric sleeve, which removes about 80 percent of the stomach, is the most commonly performed bariatric surgery. In addition to restricting the amount a patient can eat, the hormones that control their hunger are also altered.
The gastric bypass, the second most common of the bariatric procedures, restricts how much a patient can eat, limits how many calories a patient’s body can absorb, and resets hormones that control hunger and metabolism, including an increase in the body’s own production of GLP-1.
One of the newest of these procedures is the single anastomosis duodenoileostomy with sleeve gastrectomy, also known as SADI-S. It involves a gastric sleeve and an intestinal bypass, which is similar to the gastric bypass, but with a few important alterations.
“There are some potential long-term symptoms a patient can develop after a gastric bypass that are specific to the anatomy created during the SADI-S,” Bruenderman says. “The other benefit of the SADI-S is you have greater weight loss than you would see in the gastric bypass. With the bypass, you are going to see on average 70 to 75 percent of your excess body weight lost in a year to a year and a half after surgery. With the SADI-S, it is 80 to 85 percent.”
Which approach to take with a patient depends partly on the patient’s body mass index (BMI). Bruenderman says patients with a BMI higher than 50 are optimal candidates for SADI-S, though many insurances do not yet cover this relatively new procedure. In those cases, patients can still pursue other surgical options or incorporate medical weight loss treatment as a preoperative adjunct. That is where the GLP-1 medications can play an important role.
“The newer generation of weight loss medications are miraculous,” Bruenderman says. “They have completely revolutionized the field of medical weight loss. Having these medications at our disposal allows me to potentially start patients with very high BMIs on a medication preoperatively to lose a little bit of weight before surgery to make their surgery safer.”
The Future of Weight Loss in Kentuckiana
Bruenderman is optimistic about the future of obesity and weight loss healthcare. She emphasizes the need for a different perspective and the importance of the patient’s mental approach to the journey.
“I encourage patients to look at this condition in the same way that you would look at cancer,” she says. “If you’re diagnosed with cancer, you have an entire team of physicians who are following guidelines to come up with a multidisciplinary treatment plan involving a combination of medical treatment, surgical treatment, radiation treatment, etc. The same should be true for obesity.”
“If you are a patient who is getting treatment for obesity from only one modality, you are not getting the best obesity treatment that exists. Obesity is a chronic condition. It has to be treated with different modalities over your entire life.”
Part of the lifelong success involves focusing on the quality of life, not the weight. Bruenderman calls them non-scale victories (NSVs), focused on how patients’ lives have changed post-surgery. For some, that might be riding a rollercoaster with their kids or getting a whole new wardrobe, and for others it might mean no longer needing to take insulin injections.
“All of these things have nothing to do with the number patients see on the scale but have everything to do with how their lives are changed,” Bruenderman says. “I get to empower people to make really significant changes in their lives. That is what I love most about my job and why I became a bariatric surgeon.”

