Endocrinologist Kupper Wintergerst, MD, and his team go the extra mile for their patients with diabetes
LOUISVILLE As the saying goes, an ounce of prevention is worth a pound of cure. While there is no cure yet for type 1 diabetes, significant strides have been made recently in understanding how to prevent — or at least delay — the onset of the disease. Kupper Wintergerst, MD, says that has led to a different approach to treating patients with diabetes.
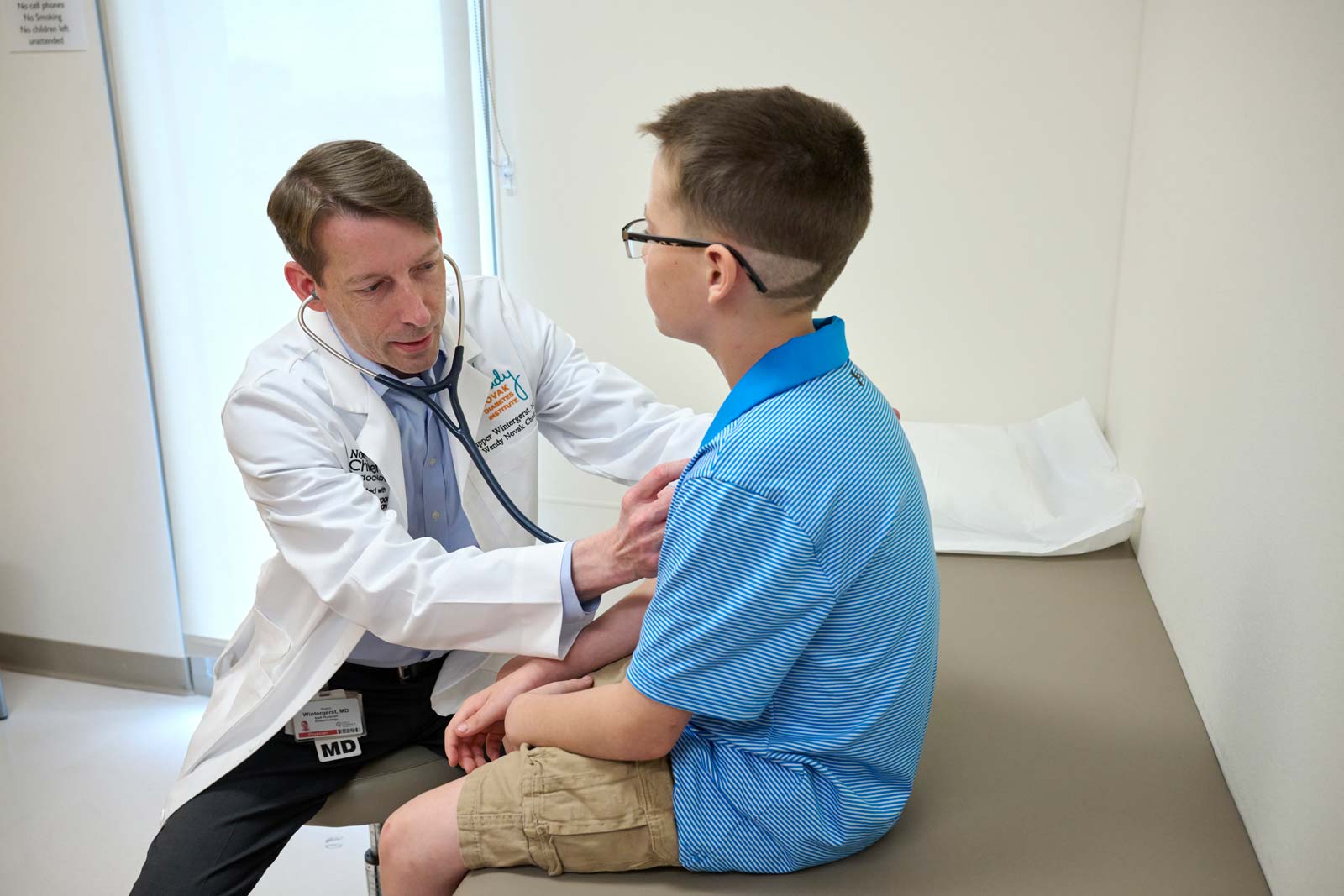
“Teplizumab, the first drug available to delay the progression of type 1 diabetes, is on the market,” says Wintergerst, who is chief of pediatric endocrinology with Norton Children’s Endocrinology, affiliated with the University of Louisville School of Medicine, and director of the Wendy Novak Diabetes Institute. “This is used in individuals whose probability is nearly 100 percent of developing type 1 diabetes in the immediate future. They not only have antibodies that are positive — evidence that their immune system is destroying their beta cells — but they also have impaired glucose tolerance, meaning their blood sugars are abnormal, but not yet at the threshold that we use for diagnosing diabetes. What if we identified people with positive antibodies but normal blood sugars and we could intervene even earlier? We could potentially delay diabetes by a decade or more. What if we could eventually use these drugs to prevent it? So it’s not a cure, it’s a prevention therapy that is another step forward.”
Prevention, not a cure, in many ways is the preferred route and likely the most achievable. “A true biological cure for diabetes will continue to be a challenge because it is a complex condition that has no one single cause. It is multifactorial; it is caused by triggers that influence your immune system and create a cascade that isn’t always down one pathway,” says
Wintergerst. “But what we can do is potentially create something that takes away the burden of diabetes, such as with islet cell transplantation. Islet cells are in the pancreas, and beta cells are a type of islet cell that produces insulin. If we were to take cells that are healthy, put them in a human who has type 1 diabetes and either give them a drug that protects those cells or create a way to encapsulate those cells to protect them from the immune system, then we could effectively make it so that someone with diabetes doesn’t need to monitor their blood sugar or take insulin because they have cells that are doing the job that their body is supposed to do. I think we will eventually get to the point where we will be able to do that type of therapy for someone who has been diagnosed with diabetes. That is on the ever-present horizon that we’re all chasing.”
Wintergerst has been chasing that horizon since he graduated from the University of Louisville School of Medicine. A native of Louisville, he graduated from St. Xavier High School and Bellarmine University. After medical school, he did his pediatric training at the University of Florida, followed by a pediatric endocrinology fellowship at Stanford University. He returned to Louisville in 2006 to join the Division of Pediatric Endocrinology at Norton Children’s and the University of Louisville. His sister, Katherine Rogers, APRN, DNP, also works at Norton Healthcare as a Vice President of Patient Care Services and Chief Nursing Officer for Norton Medical Group and Norton Cancer Institute.
Patients, Administration, Teaching and Clinical Trials
Currently, Wintergerst sees patients on Mondays and Tuesdays in the Novak Center for Children’s Health, while his primary work is in clinical research through the Norton Children’s Research Institute. Wintergerst’s administrative duties include overseeing the activities of faculty and the physicians who also have appointments. As if that weren’t enough, he also continues to teach as a professor of pediatrics at the University of Louisville School of Medicine.
“Part of our responsibility in academic medicine is to educate the physicians of the future,” Wintergerst says. “We have medical students, medical residents, and fellows in all areas, including endocrinology, that rotate through our practice for their endocrine training, which includes direct patient care experience, didactic teaching sessions, and formal lectures.”
Wintergerst says the ongoing research and advances in diabetes prevention and treatment has helped create more student interest in endocrinology.
“When students see how valuable each of the disciplines are to the care of a single child and their family, it really does create that excitement and there’s more exposure to our specialty,” he says. “Diabetes care options have dramatically changed from a simple, and very limiting, insulin management plan that was complicated by an inability for the patient to

deviate from a set schedule if they wanted to achieve even reasonable blood sugar control. Now, the technology and the different therapeutic options that are available allow us to tailor our diabetes management to the child’s life rather than the other way around. Medical students see that they can make a meaningful difference in a child’s life and the more they can do for a patient and family as a healthcare provider, the more excited they are.”
The Wendy Novak Diabetes Institute serves everyone with diabetes within Norton Healthcare and Norton Children’s, totaling more than 100,000 patients. Specifically, in pediatrics, the team serves endocrinology patients up to 21 years of age, and the Institute serves diabetes patients up to age 26. Wintergerst says there are more than 10 different forms of diabetes, with the most common being type 1 diabetes and type 2 diabetes.
A Statewide Problem and Solution
Wintergerst says that many factors are responsible for the high rate of diabetes in Kentucky.
“There are communities that do not have access to healthcare providers,” he says. “People are driving one, two hours for care. Endocrinology, unfortunately, is one of those areas of health care that is underserved. We have areas within cities and in rural areas where people do not have easy access to fruits and vegetables and healthy choices that are affordable. It’s easy for me to say to a patient, ‘You need to include more vegetables in your diet, just go and buy them.’ But if they can’t afford them, then that can be an insurmountable challenge. Even with immediate access to cheap vegetables, change does not happen quickly because our eating habits are often generational. If families have been eating a certain way because that is all they’ve had available for generations, then it will take more than a single grocery store offering cheaper, healthier food options to affect rapid change within a community, much less an individual. We have to keep thinking bigger.” Wintergerst knows change takes participation and teamwork from all angles, but he is determined to play his part to make it happen.
“Somewhere within my job title, I think, is working to change the future in the world of diabetes,” he says. “We had about a few hundred patients when the diabetes center was first formed and then we built it and they came. And they came from further and further and further away because they knew that if they committed to driving two or three hours to come to Louisville, that their children and their families would live longer, healthier, active lives. All because of our amazing team and how much they care about our kids.”
Wintergerst says that being active is essential for patients with diabetes.
“When it comes to diabetes, we’re trying to get patients out there for the first time if they’ve been fearful of participating in exercise,” Wintergerst says. “So how do we make it so that every athlete, every child, and adult who just wants to walk at the mall or the park or play soccer, or whatever it might be, how do we empower them, build their confidence so that they know how to safely do all those things? That’s what our sports program, the Christensen Family Sports and Activity Program, does.”
Connection and Education
Connecting patients to resources and educating them about their care and management is one of the reasons Wintergerst was interested in endocrinology.
“One of the things that drew me to endocrinology is that we often see patients for many, many years because when they come to us, a high percentage of them have chronic health conditions that we do not just diagnose and then send them on their way,” he says. “We manage them over the years as they grow and develop into healthy adults. When we manage diabetes, we actually have to delve into the daily lives of our patients. So we go

beyond that relationship, that patient-provider, that patient-family relationship, to a point where we know what sports they play and how well they did in the tennis tournament last week, and whether they have a dog or do they horseback ride or do they like to travel? It’s valuable because it helps to determine what we’re going to do to more appropriately manage their health condition.”
During this season of graduations, Wintergerst is particularly mindful of the relationships he and his team develop with their patients.
“Sometimes it’s amazing to realize that you have been part of, and one of the reasons why, that child has been able to graduate high school and get their first job, or graduate college or even complete graduate school, because you and your team were a part of their lives,” Wintergerst says. “That is often what drives us. We’re taking on burdens from those families and we’re taking them into ourselves. But in the end, those relationships are the reason that we continue. We’re passionate about what we do.”
Research and Relationships
Wintergerst is also passionate about research and finding better ways to prevent diabetes. He hopes that screening, and medications such as Teplizumab, will help identify and prevent diabetes and other diseases.
“What we aim to do is to figure out how can we create public health initiatives around antibody screening,” Wintergerst says. “In the future, if we identify someone with an auto-immune condition early through public health screening programs, we can actually intervene and change their future. That’s what public health screening is all about.”
These advances are not happening overnight, which means Wintergerst and his team must continue their daily work to treat the patients and their families dealing with diabetes. He endeavors to listen and learn and understand their needs, even if it takes a little extra time.
“I try to treat my patients, these young adults and their families, like they’re mine, like they are my child or this is my family,” he says. “And so, when I think about what I would want for my child, that is exactly my focus. Not just when I am considering treatment options, but also how much time I spend with them. If this is a family that is struggling, I know that if I were struggling or if my child was struggling, how much I would appreciate someone spending that extra minute. There are kids and families that are having to manage something that can be devastating. And so how do we make it so that they can live happier too, not just healthier?”
With his teaching, research, hospital calls, and patient care, how does Wintergerst justify taking that extra time with each family? The answer is quite simple.
“We love our patients, we want them to be successful, we want them to have healthy lives,” he says. “That’s why you go above and beyond. Above and beyond doesn’t end at 5:00.”
